CLINICAL CONTEXT
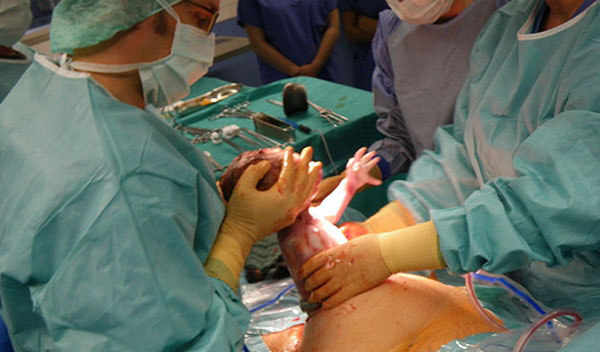
The proportion of cesarean deliveries has increased in the United States, reaching a level of 32% of all deliveries in 2007. This trend is troubling for many reasons, but most clinicians do not consider alterations in gut flora during childhood as an important problem associated with the higher rate of cesarean deliveries. Perhaps it is time that they should.
The authors of the current study explain that alterations in gut flora are the leading theory of why a history of cesarean delivery may promote higher rates of childhood obesity. Children delivered vaginally have been demonstrated to have different types of intestinal flora vs children delivered via cesarean, and this alteration may not only explain a propensity toward obesity among children delivered via cesarean but may also explain higher rates of asthma and allergy.
Nonetheless, no prospective research has examined how the mode of delivery affects rates of childhood obesity. The current study by Huh and colleagues addresses this issue.
STUDY SYNOPSIS AND PERSPECTIVE
Cesarean delivery doubles the risk for childhood obesity, according to a prospective cohort study published onlineMay 23 in the Archives of Disease in Childhood. The reason may be different intestinal bacteria than those acquired during vaginal birth.
Susanna Y. Huh, MD, MPH, from the Department of Pediatrics, Harvard Medical School, and Division of Gastroenterology and Nutrition, Children’s Hospital Boston, Massachusetts, and colleagues evaluated 1255 mother-child pairs attending 8 outpatient maternity practices in the Boston area between 1999 and 2002. The researchers weighed and measured children at birth, 6 months, and 3 years, adding triceps and subscapular skinfold thicknesses at the 3-year check. Mothers submitted questionnaires at 1 and 2 years postpartum.
Approximately one quarter of deliveries were surgical (22.6%; 284 children). These women weighed more than the women delivering vaginally; their babies weighed more, accounting for gestational age; and the mothers did not breast-feed for as long as the women who delivered vaginally.
Nearly 16% of children delivered surgically became obese compared with 7.5% of those born vaginally. Birth by cesarean delivery was associated with higher odds of obesity at age 3 years (odds ratio, 2.10, 95% confidence interval [CI], 1.36 – 3.23), higher mean body mass index (BMI) z-score (0.20 units; 95% CI, 0.07 – 0.33), and higher skinfold thicknesses (0.94 mm; 95% CI, 0.36 – 1.51), with adjustments for birth weight, prepregnancy maternal BMI, and other factors. The results are consistent with those of a smaller, retrospective study of 3- to 6-year-olds in China.
An explanation for the different risks for obesity with the 2 birth methods may lie in the microbiome, the communities of microorganisms that colonize the human gastrointestinal tract. Each method may introduce different bacterial species.
Gut bacteria affect the efficiency of energy extraction from nutrients and may stimulate cells to boost insulin resistance, inflammation, and fat deposits, the authors write. Specifically, higher numbers of Firmicutes and lower numbers of Bacteroides colonize the guts of children born by cesarean delivery. Other studies have shown this pattern in the gut microbiomes of obese individuals.
Limitations of the study include self-reporting of prepregnancy weight and the generalizability of the highly educated and earning study population to the general population.
The researchers suggest further studies to confirm the association between cesarean delivery and obesity and to further investigate the gut bacteria hypothesis. An alternative explanation may be effects of antibiotic prophylaxis given during cesarean delivery on intestinal bacteria.
The risk for obesity did not differ between planned and emergency cesarean deliveries, suggesting that bacteria acquired when membranes rupture are not a factor in elevated obesity risk, the researchers write.
One in 3 deliveries in the United States is surgical. Previous studies have associated cesarean delivery with increased risk for asthma and allergic rhinitis. “A mother who chooses caesarean delivery…should be aware of potential health risks to her and her baby, including childhood obesity,” the researchers conclude.
The study was supported by grants from the National Institutes of Health. The authors have disclosed no relevant financial relationships.
Arch Dis Child. Published online May 23, 2012. Abstract
STUDY HIGHLIGHTS
- Study participants were women attending their first prenatal visit before 22 weeks’ gestational age in Boston. Women with multiple pregnancies were excluded from participation.
- Women underwent a thorough examination, and their children were evaluated at ages 6 months and 3 years for height and weight. Researchers also measured the child’s subscapular and triceps skinfold thickness at age 3 years.
- 1579 women were eligible for study participation, and data were available for 1255 mother-child pairs.
- The primary study outcome was the relationship between cesarean delivery and the rates of overweight and obesity at age 3 years. Obesity was defined as a BMI of 95% or more adjusted for age and sex, and overweight was defined as an adjusted BMI of 85% or more.
- The main study results were adjusted to account for maternal demographic factors; anthropometric data; gestational weight gain; maternal smoking; maternal glucose tolerance; and childcare factors, including breast-feeding, the child’s diet, and the child’s degree of sedentary activity.
- Of the 1255 deliveries, 22.6% were by cesarean delivery. Maternal BMI and birth weight for gestational age were higher among cesarean deliveries, and babies delivered via cesarean had shorter durations of breast-feeding vs babies delivered vaginally.
- Higher maternal body weight and higher birth weight were associated with increased risks for obesity at age 3 years.
- The mean BMI z-scores at age 3 years for children delivered via cesarean and vaginally were 0.67 and 0.39, respectively. The respective rates of overweight were 18.9% and 16.7%, and the respective rates of obesity were 15.7% and 7.5%.
- The adjusted odds ratio for obesity at age 3 years associated with cesarean delivery was 2.10 (95% CI, 1.36 – 3.23). However, cesarean delivery did not increase the risk for overweight at age 3 years.
- Cesarean delivery was most associated with a higher risk for childhood obesity among women with a prepregnancy BMI of 25 kg/m2 or less.
- Cesarean delivery was also associated with a higher BMI z-score and the sum of subscapular plus triceps skinfold thickness.
- The difference in the rates of obesity and increased skinfold thickness was scarce in comparing planned vs unplanned cesarean deliveries.
CLINICAL IMPLICATIONS
- The leading theory of how cesarean delivery may promote higher rates of childhood obesity is an alteration in gut flora among children.
- In the current study by Huh and colleagues, cesarean delivery was independently associated with higher risks for obesity and increased skinfold thickness during early childhood.
News Author: Ricki Lewis, PhD
CME Author: Charles P. Vega, MD, FAAFP
 Whitehouse Pharmacy Whitehouse Pharmacy
Whitehouse Pharmacy Whitehouse Pharmacy